Everyone talks about cavities from bacteria and lazy brushing, but there’s this sneaky parallel problem eating away at your teeth with zero germs involved. Clinically, it’s tooth erosion, a pure chemical attack where acids directly melt the dense dental tissues. Regular cavities need bacteria feasting on sugars to spit out acid byproducts, but erosion hits different. It’s repeated direct exposure to acidic environments that rip essential minerals straight off the tooth surface, no middleman.
Enamel’s basically a fortress of hydroxyapatite crystals packed insanely tight—the hardest substance your body’s got, built to take brutal chewing punishment. Mechanically tough? Absolutely. But chemically, it has this glaring weakness. When oral pH falls below the critical 5.5 threshold, the surrounding environment becomes highly corrosive. Acid molecules break the chemical bonds that hold calcium and phosphate ions in the enamel’s structure.
The surface softens instantly, turning the microscopic structure vulnerable to everyday wear—think food grinding, coarse biting, and even gentle toothbrush friction wearing it down fast.
Dietary Acids You Sip (or Eat) Every Single Day
External acid sources rule modern habits, no question. Think beverages engineered for max acidity: carbonated sodas, sports drinks, and even those “healthy” sparkling waters. They load up citric acid or phosphoric acid for flavor pop and long shelf life. Problem? They are consumed continuously throughout the day. Your mouth can’t neutralize naturally—enamel stays trapped, demineralizing around the clock, never catching a break.
Same deal with natural stuff. High citrus fruit intake—lemons, oranges, and grapefruits—or vinegar dressings and chewable vitamin C supplements. All pack potent erosive punch. Consumption style matters big time here. A straw safely funnels liquid past the front teeth, but what about swishing it around or holding it in your mouth? That bathes every surface in maximum exposure, accelerating damage way worse. Small daily choices snowball over months.
Your Body’s Own Brutal Internal Acid Attacks
Biological triggers hit equally hard, sometimes meaner. Gastric acid clocks in at pH 1.5-3.5 typically—orders of magnitude more vicious than any soda. Individuals suffering from gastroesophageal reflux disease (GERD) involuntarily reflux this beast into their mouths, often at night while lying down. Salivary flow naturally tanks during sleep, so acid pools undiluted against palatal surfaces of upper teeth for hours on end.
Eating disorders with frequent vomiting expose teeth to identical extreme acidic baths repeatedly. Repeated exposure to stomach acid causes the inner enamel layers to dissolve quickly, a process that happens much faster than if it were only caused by food. Moreover, internal factors are often harder to notice.
Physical Signs As Erosion Chews Through Structure
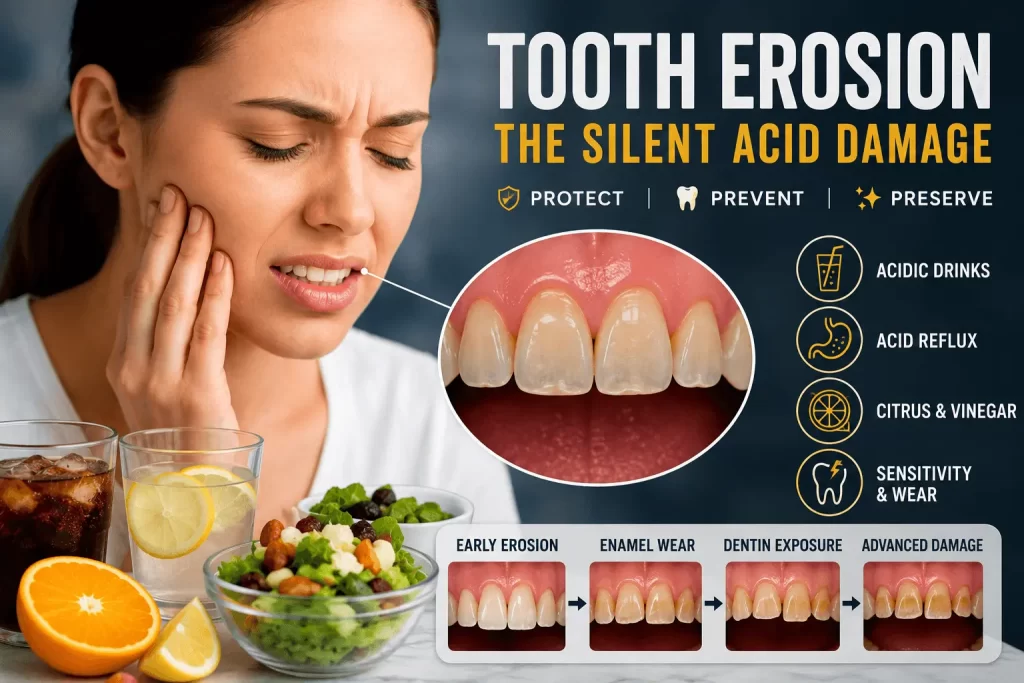
Spotting chemical wear takes practice; early stages are usually hurt-free. Teeth develop slick, glossy polish first—the outermost micro-layer dissolving away. Advances to characteristic cupping: small indentations pitting molar biting surfaces. The cutting edges of front teeth become significantly thinner, acquiring a translucent, glassy appearance that readily chips when subjected to even moderate biting forces.
The underlying dentin layer’s naturally yellowish hue shines through as white enamel casing thins. The entire tooth darkens and looks severely discolored overall. Enamel barrier fully breached? Microscopic dentinal tubules now face oral environment directly. Cue reliable, sharp hypersensitivity—thermal changes and sweet foods trigger intense zings immediately.
Practical Steps to Actually Stop (and Reverse Early) Damage
Halting progression means behavioral tweaks over just brushing more often. Huge mistake: attacking teeth mechanically right after acidic exposure. Temporarily softened enamel scrubs away worse under bristles. Professionals drill teeth: wait 30-60 minutes minimum post-acid hit. Salivary calcium has time to naturally remineralize and reharden the surface first.
Specialized intervention essential for root-cause diagnosis and protection. High-concentration fluoride varnishes and bonded composite resins rebuild defense. Established networks like Dentprime link to trained restoratives running precise protocols, mapping exact structural loss severity through targeted diagnostics.
Long-term victory demands a three-pronged attack: neutralize acid sources completely, chemically reinforce surviving enamel, and physically restore compromised anatomy via fillings or bonding. Move fast before irreversible pulpal nerve damage sets in. Worth the effort—your teeth last decades longer.

Sumit Rajput
May 17, 2026 at 5:54 amVery informative article. Cancer recovery is not only about treatment procedures; emotional support, nutrition, and healthy lifestyle habits also play an important role. Many patients today explore Ayurveda Cancer Treatment in india for complete wellness support during recovery. Awareness and patient-focused care can help improve overall healing experiences. Great insights shared here!